You’ve felt it. That tightening in your chest when you look at your renewal statements. The carriers are squeezing margins, the “easy” Medicare sales are becoming a commodity war, and you’re working twice as hard just to maintain the lifestyle you had three years ago.
Most agents respond by “running more laps”—buying more leads and burning more gas. But the elite 1% of producers aren’t running harder; they’re looking at the math differently. They’ve realized that the most valuable real estate in the industry isn’t a new lead… it’s the Medicare Supplement conversation you’re already having. These elite producers understand that most of their clients could benefit from our short term home health care cross-sell strategy.
The New Mechanism
At Senior Benefit Services, we don’t believe in “grinding” through a commission slump. We believe in the Net-Zero Cross-Sell.
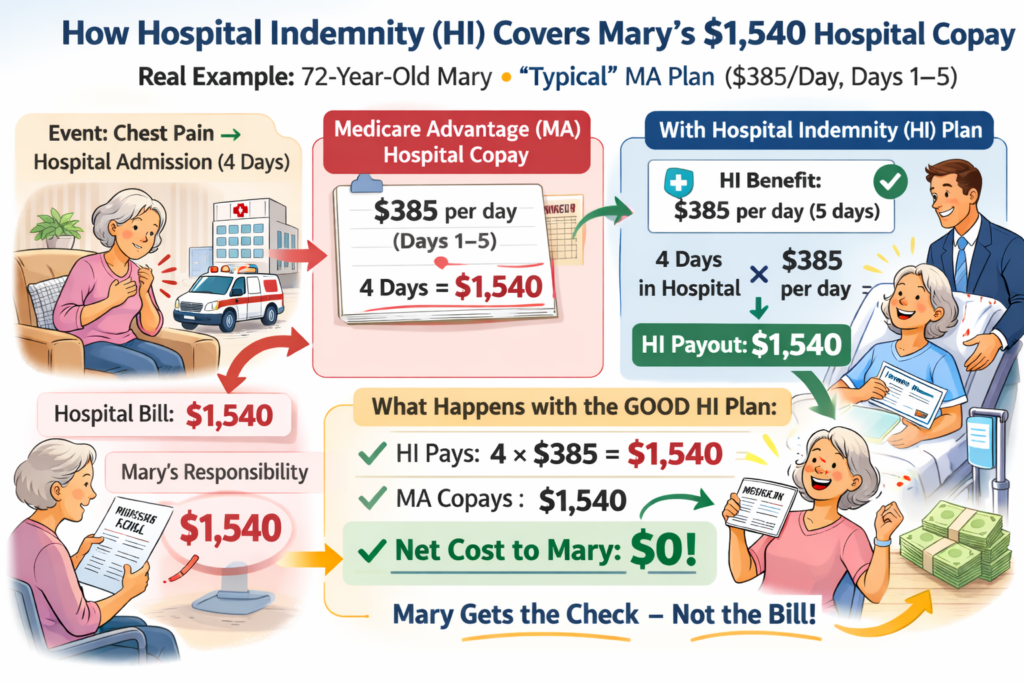
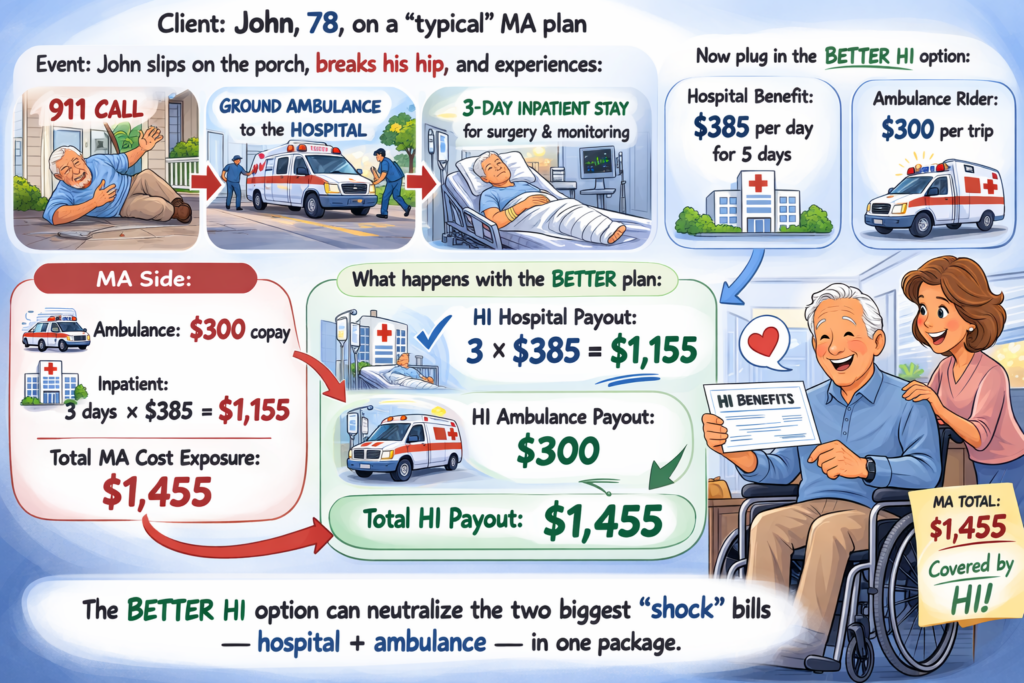
The secret lies in Short Term Home Health Care (STHHC). While most agents ignore this product, the heavy hitters are using a specific “Prescription Offset” strategy. Because certain carriers offer prescription reimbursement benefits that can actually equal or exceed the plan’s premium, you can offer your client massive protection—Home Health Care, Nurse Aide coverage, and Therapy—for a net cost of essentially zero.
Why do your clients need a STHHC plan? Medicare provides very little coverage for the most needed services that home health care agencies and aides perform. Additionally, to qualify for those services, your client has to meet specific criteria. If you are not familiar with what Medicare will and will not cover, the National Council on Aging did a nice article breaking it down.
The “Prescription Offset” – Why Your Clients Will Say Yes Before You Finish the Sentence
In a market where every penny counts, your clients are terrified of rising drug costs. When you show them a plan where the prescription reimbursement pays them back their premium, the “sale” disappears. It becomes a transfer of risk that costs them nothing.
-
The Client Wins: They get a safety net for home recovery that Medicare often leaves gaps in.
-
The Agent Wins: You secure a high-quality cross-sell commission that stabilizes your book of business against Medicare Supplement rate hikes.
Stop Being a “Quote Machine” and Start Being a Strategist
Independent agents often fail because they are treated like “order takers” by their FMOs. You get a contract, a pat on the back, and a “good luck.”
Senior Benefit Services is different. We provide the specific scripts and carrier nuances to identify which clients qualify for the “Net-Zero” offset. We show you how to transition from a Medicare Supplement review into a STHHC conversation without sounding like a “salesman.”
Why Partner with Senior Benefit Services?
-
The Blueprint: We don’t just give you a product; we give you the “Big Hook” strategy.
-
The Support: Our marketing department is staffed by people who actually understand the senior market—not just “tech guys.”
-
The Independence: You keep your independence, but you gain the institutional knowledge of a powerhouse.
- The Experience: All our methods are actually tested prior to being rolled out to independent agents.
What Should You Do?
You can keep watching your renewals dwindle, or you can pivot to the strategy that is currently saving the margins of the top producers in the country. Let us show you the specific carriers and the “Prescription Reimbursement” math that makes this the easiest “Yes” in your portfolio. Contact our Marketing Department today at (800)924-4727 for the “STHHC Blueprint”!